It’s time to fix the glaring gaps in death data and drastically improve measures to keep the coronavirus out of nursing homes.
As we hit a gruesome milestone — 100,000 reported deaths from the novel coronavirus in the United States — we must focus on the single most important part of the response: saving the most lives.
The SARS-CoV-2 virus is likely to kill more than 1 million people worldwide by the end of this year, and 60 million people will die this year from other, often preventable causes, as they do every year. As we confront the most devastating infectious disease threat the world has faced in a century, unless we are more careful, there will be many more avoidable deaths, not just from Covid-19 but also from the disruption it causes.
If there’s one constant in the varying effectiveness of responses in different cities, states, and countries, it’s the tight correlation between how fully political leaders are guided by and support public health (for example, in Singapore, Germany, New Zealand, Seattle, and elsewhere) and how well they prevent their people from being killed by the virus.
To save as many lives as possible, both from the coronavirus and other causes, public health specialists must guide and political leaders must fully support five things at the core of public health.
1) Fix the glaring gaps in data about deaths
Although deaths are not an early indicator of the spread of the coronavirus and other health trends, tracking death rates is crucial to understanding and counteracting the impact of the pandemic. Tracking deaths identifies increases from the virus missed by testing and tracking systems and provides an early warning if deaths from other conditions increase.
What gets measured can be managed, and so every US state and every country must report all-cause mortality every week. Many higher-income countries can start weekly reporting by age group compared with historical levels, as Switzerland and others have done.
:no_upscale()/cdn.vox-cdn.com/uploads/chorus_asset/file/20000831/Screen_Shot_2020_05_26_at_1.20.55_PM.png)
Even in the United States, this information isn’t readily available, and in places ranging from New York City to Georgia, public health leaders have had to resist pressure from political leaders to hide this key data.
We need to change the expectation so that we learn the death rates every week, in every community — both deaths caused by the coronavirus and all deaths. In lower-income countries where basic vital registration systems are often weak or lacking, this will require training, supporting, and paying community health workers and hospital registrars and also improving the capacity to collect, analyze, and disseminate real-time data. Last week, our organization, Resolve to Save Lives, joined the World Health Organization and others in releasing practical guidance on how countries can do just that.
In the US, this increase in deaths from other conditions, which results from the pandemic’s disruption, could come in the form of more heart disease deaths among those who didn’t seek care during the pandemic. At the height of the pandemic, a colleague in a New York City emergency department commented to me, “We’re seeing no angina.” It’s likely that patients with heart attacks avoided care for fear of contracting the coronavirus.
RELATED
The coronavirus crisis is leading to an immunization crisis
In Africa, meanwhile, falling immunization and malaria treatment rates could cause millions of preventable deaths. These trends can be found early — and further deterioration prevented — with rapid mortality surveillance.
2) Protect our health care workers to keep our health care systems functioning so they can prevent both coronavirus and non-coronavirus deaths
It is appalling that more than 100,000 health care workers have been infected with the novel coronavirus. The health and economic consequences of losing health care workers and overwhelming health care facilities are catastrophic.
This does not have to be. I began my public health career documenting and stopping the spread of multidrug-resistant tuberculosis in hospitals; it is possible to make health care much safer.
Singapore has had few if any health care workers infected by the virus at work — not thanks to high-technology interventions, but due to sensible, meticulous attention to protocols. Protective equipment is important, but comprehensive and well-implemented infection prevention programs are the most effective ways to protect health care workers and patients.
Only if health care workers are and are known to be safe will we be able to prevent avoidable deaths from people infected with the novel coronavirus and also prevent increases in mortality from other conditions that result from overwhelmed health care systems.
3) Preserve non-coronavirus health care
In New York City, between mid-March and mid-May, there were more than 4,000 “excess” deaths — deaths that may have been but are not known to have been related to the coronavirus. It’s likely that many people died from non-coronavirus causes because they did not seek care, for example for heart disease, which is the leading cause of death in the US.
RELATED
Africa has so far been spared the worst of the coronavirus. That could soon change.
Avoiding an increase in non-coronavirus deaths is a particularly urgent priority in Africa. If we don’t take steps to preserve care, over the coming years more than 10 million people in Africa could die from malaria, tuberculosis, HIV, vaccine-preventable diseases, and other causes due to the pandemic’s disruption of health care systems. Yet the age structure — only 4 percent of Africans are over age 65 — means that the proportion of coronavirus infections that are fatal will be far below 1 percent: closer to the seasonal flu than to the devastation seen in other parts of the world.
If we fail to preserve the programs that address preventable killers, the number of people who die from the coronavirus directly might be a small fraction of those killed by other diseases because of the disruption the pandemic causes. Donor agencies, international organizations, and governments themselves must keep non-coronavirus health care going, with telemedicine, longer-term prescription refills, safer facilities, and bolstered primary and preventive care.
4) Protect the most vulnerable
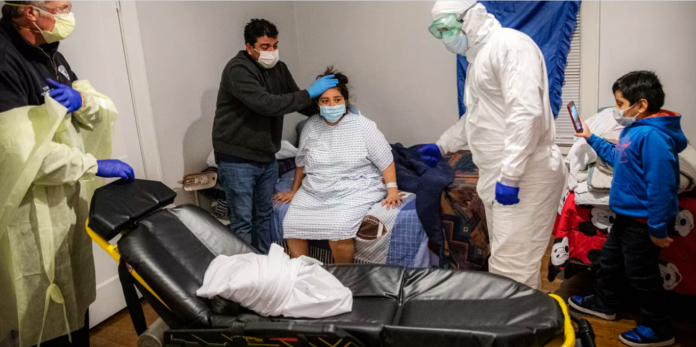
One-third of the US coronavirus deaths have occurred in nursing homes, revealing that facilities for the elderly will be coronavirus death traps until we drastically improve efforts to keep the virus out, find it fast when the first staff or residents become infected, and stop outbreaks from spreading.
The US Centers for Medicare and Medicaid Services (CMS) has made a good start requiring an end to nonessential visitors, but regulators, payors, and nursing home administrators will all need to keep the virus out with strict policies. These include universal wearing of masks, limited visitors, and extensive testing. Nursing homes need to find the virus fast with rapid and repeated testing, and they need to stop outbreaks before they spread widely with rapid-response teams and test-based strategies. We need to identify and protect the highest-risk facilities — not just nursing homes, but also prisons, homeless shelters, and factories, and the highest-risk individuals, including the elderly and those with underlying conditions.
5) Balance saving lives with preserving livelihoods
Health versus the economy is a false dichotomy. Poverty increases ill health, and until people are confident, they will not resume economic activities.
Yogi Berra asked, “If people don’t want to come to the ballpark, how are you going to stop them?” Unless people feel safer working, dining, or shopping, they won’t venture out for those activities.
The coronavirus will cause the first increase in global poverty in more than two decades. In a recent survey in Africa, half of respondents estimated they would run out of money and food in a week or less.
RELATED
Contact tracing, explained
Every country needs to find the balance, and this may mean allowing economically important activities to begin even before all of the ideal disease control systems are in place. This can only happen if we better protect health care workers, shield the most vulnerable, and redesign to reduce risk. In most places, most economic disruption from the pandemic isn’t from lockdowns, but from fear — much of it rational — that everyday activities could kill us or our loved ones.
It’s not a “guns or butter” dilemma. We can save the most lives and protect our economy most effectively by urgently strengthening public health and emerging as soon and as safely as possible, focusing on the most important societal activities first. This means widespread use of face masks, hand-washing, staggered shifts, telework, and prompt contact tracing to prevent cases from becoming clusters, clusters from becoming outbreaks, and outbreaks from forcing another retreat into our homes.
The British epidemiologist William Farr wrote, “The death rate is a fact; anything beyond this is an inference.” Weekly mortality tracking can guide a response that rapidly identifies and prevents further increases in coronavirus and non-coronavirus deaths. Only focused and intensive action will prevent another 100,000 deaths in our nursing homes alone.
As future waves of the virus hit, we need to be ready to adapt rapidly to reduce spread, stop outbreaks, and protect the vulnerable. In every step we take, we must first remember: Illness and economic damage are reversible. Death is not.
Tom Frieden is a senior fellow for global health at the Council on Foreign Relations, CEO of Resolve to Save Lives (an initiative of Vital Strategies), former director of the US Centers for Disease Control and Prevention, and former commissioner of the New York City Health Department. Follow him @DrTomFrieden on Twitter and Instagram.
Reference Link:
https://www.vox.com/2020/5/26/21270703/coronavirus-deaths-us-world-covid-19-nursing-homes